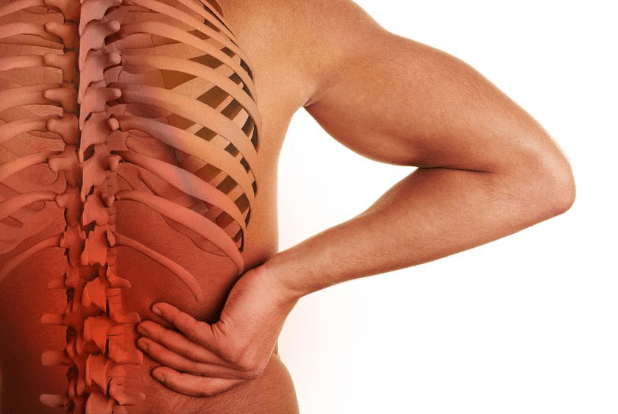
Spinal Osteoarthritis
Low back discomfort affects up to 80% of the population. In osteoarthritis, cartilage degeneration is a frequent source of low back discomfort (tissue covering the joint surfaces at the ends of bones)
Pathology
Healthy cartilage cushions the bones when they move against one other in normal
joints, allowing them to move freely. When the cartilage lining the facet joints
(vertebral joints) breaks out, it allows the bones to rub against one other,
causing spinal osteoarthritis. Facet joints and vertebrae develop osteophytes,
or tiny bony growths commonly known as bone spurs, as a result of an effort to
reestablish stability in the joint. There is a gradual loss of flexibility and
stiffness in the spine as we age. There have been cases when the osteophytes in
the spine have grown big enough to obstruct the nerves flowing through the foramen
magnum or spinal canal (spinal stenosis and foraminal stenosis). Osteoarthritis and
stenosis are connected medical conditions, however stenosis is a distinct medical
problem. As with degenerative disc disease (a slow degradation of discs between vertebrae),
osteoarthritis may also be mistaken for degenerative disc disease. There is no clear link
between aging and osteoarthritis. For example, it may be caused by overuse of a joint
or other mechanical stressors such as repeated motions or injury. Inheritance also has
an impact.
Symptoms
Pain and stiffness are the primary symptoms, which worsen with time. Pain and stiffness are the first symptoms that appear after a prolonged period of inactivity. Physical exercise and extended sitting might exacerbate the discomfort in the latter stages of the illness.
Diagnosis and Treatment
The source of back pain is an important factor in determining the best course of therapy. An x-ray or other imaging study of the spine may be ordered by your doctor to help determine the source of your back discomfort. Your doctor will ask about your medical history and do a physical examination before making a diagnosis. In order to alleviate pain, preserve joint mobility, and decrease the course of arthritis, treatment focuses on these three areas. As a first step, a treatment plan should be devised that incorporates exercise, medicine, and measures to preserve joints. Additionally, you might be sent to an orthopedic surgeon or a rheumatologist or Physiotherapist. Back osteoarthritis may be treated using a variety of methods:
- Education: the best way to avoid back problems is to know their causes.
- Low-impact exercise (walking, biking, swimming) improves muscle strength and flexibility, helping to support the spine. A gradually increasing program is recommended.
- Rest during active inflammation.
- Heat and cold to reduce inflammation.
- Adequate back support (firm mattress, supportive chair).
- Weight control.
- Complementary treatment. This includes Physiotherapy and Massage therapy.
- Pain relievers (such as acetaminophen, aspirin, and other nonsteroidal anti-inflammatory drugs), topical creams, and opioids (such as codeine).
- Injections targeting the epidural space (narrow space between membranes covering spinal cord and wall of spinal canal), the facet joints or blocking specific spinal nerves.

How Physiotherapy Can Help With Osteoporosis?
Physiotherapy has been demonstrated to be useful in the treatment and management of osteoporosis. Pain management measures, posture and balance improvement, as well as strengthening of muscles and bones, are all helped by it.
Strength training and low-impact exercises may reduce fracture risk by strengthening bones. Strength training and other forms of intense exercise are often avoided by those with osteoporosis due to their perceived risk of fractures. Any physiological system's performance can only be improved by being subjected to a load that is much greater than the usual. Increasing strength requires that the skeleton be subjected to daily stresses that are larger than those it is capable of withstanding. Your physiotherapist will work with you to devise an exercise plan that will help you improve your general stability and strength. Fall and fracture risk will be reduced as a result of the activity strengthening the bones and muscles.
Physiotherapy may also help reduce the likelihood of a fall via exercises that improve coordination and balance. Balance may be improved by doing these exercises while walking around dangers, in tight places, or on unsteady surfaces. Patients will be able to retain their equilibrium when confronted with external stimuli.
Physiotherapists also seek to improve posture with strengthening and moderate range-of-motion exercises. The increasing flexion of the thoracic spine causes gradual fractures and wedging of the thoracic vertebrae. Poor posture exacerbates the problem. Exercise may help strengthen the upper back and core, which in turn improves posture.
There is no one-size-fits-all workout programme for persons with Osteoporosis. Based on a medical examination of muscular strength, fracture risk, degree of physical activity, range of motion, gait, fitness, and balance, each programme for the particular patient should be developed.
Physiotherapists have specialized training in re-enablement and evaluation. Evidence-based guidance, education, and exercise programmes may help avoid falls, decrease the fear of falling, raise self-confidence, and improve balance.


Direct Insurance Billing
Phoenix Physio Clinic is pleased to offer Direct Billing to the majority of Canadian insurance companies in Ontario. Once you provide us with your extended benefits insurance information, we can submit your treatment costs for direct reimbursement, saving you time and reducing your out-of-pocket expenses. We offer this service at no extra charge. The insurance companies use the phrase "direct billing" to describe when a service provider bills a client directly. Healthcare providers may charge an insurance company for services they perform directly, such as physiotherapy, massage therapy, chiropractic or naturopathic doctor, by directly charging the insurance company. It relieves the patient of the burden of completing all of the necessary paperwork. In other words, it simplifies the task of submitting insurance claims.

How Physiotherapy Helps with Knee Pain
The knee joint is one of the most active joints in the human body, which implies that knee discomfort is a typical occurrence. It has the power to sabotage even the most mundane aspects of everyday existence. It only has the ability to do two things: flex and extend. Bones, cartilage, tendons, and ligaments make up the intricate structure, all of which are prone to damage, injury, and degeneration. Physiotherapy is one of the quickest and safest methods to regain your strength and get back on the road to recovery if you are suffering from knee discomfort.

Guide To Golfer's Elbow
Medial epicondylitis is commonly called golfer's elbow or thrower's elbow. Inflammation, discomfort, and irritability occur in the tendons on the inside of the forearm, resulting in this condition. Golfer's elbow is caused by overuse of the hand, wrist, forearm, and elbow. People with this problem are often seen to be swinging a golf club or other things repeatedly. In addition to using a computer or doing yard labour, this might lead to the condition. It's especially dangerous for athletes who do a lot of overhead work, as well as for carpenters and plumbers. In males, golfer's elbow is more frequent beyond the age of 35 than it is in younger ones. Unlike tennis elbow, it is not as frequent (lateral epicondylitis). For those suffering from medial epicondylitis, a physiotherapist at Phoenix Physio Clinic can assist alleviate discomfort and increase the elbow's range of motion and strength.

What Is Dry Needling?
It's possible that you've heard about dry needling and wondered what precisely it is or whether it's a therapy that may benefit you. Even though dry needling's name may seem eerie, it is safe, non-invasive, and often helpful in treating musculoskeletal conditions. Physiotherapists who are trained and qualified in dry needling may provide the treatment. Neuromuscular discomfort and movement limitations may be alleviated by using a small monofilament needle that penetrates the skin and addresses underlying trigger points in the muscles. What is a "trigger point"? It's a local contraction or tight band of muscle fiber that disrupts function, restricts range of motion and causes discomfort or soreness in the affected area. Increasing blood flow and decreasing both local and referred pain are all possible outcomes of dry needling a damaged muscle or trigger point.

All You Need to Know About Tennis Elbow
Inflammation of the tendons that connect the forearm muscles to the outside of the elbow is known as tennis elbow. Overuse of the forearm muscles and tendons, as well as those surrounding the elbow joint, is a common cause of this condition. Lateral elbow discomfort or lateral epicondylitis, which is not necessarily connected to tennis, is sometimes known as "tennis elbow." Repetitive muscular usage is a common cause of tendonitis in tennis players. Tennis elbow affects half of all tennis players at some point in their careers. Approximately 1 to 3 percent of the population in Canada is estimated to suffer from tennis elbow (Canada). Between the ages of 30 and 50, it is most common. A source that you can trust.

Return to play after treating acute muscle injuries in elite football players.
Return to play after treating acute muscle injuries in elite football players. 2021-06-15 Morgan JPM, Hamm M, Schmitz C, Brem MH. Return to play after treating acute muscle injuries in elite football players with radial extracorporeal shock wave therapy. J Orthop Surg Res. 2021 Dec 7;16(1):708. doi: 10.1186/s13018-021-02853-0. PMID: 34876172; PMCID: PMC8650394.
Dose-related effects of radial extracorporeal shock wave therapy for knee osteoarthritis: a randomized controlled trial
Over 13.000 DolorClast® shock-wave devices are installed worldwide and are continuously employed in conducting scientific research. In fact, with 34 out of 62 randomized Controlled Trials listed in the PEDro database, the DolorClast® devices are used in more studies than any other ESWT device. In this list of clinical evidence, the following study triumphs, due to the fact that it demonstrates the extent to which treatment outcomes are dose-dependent.

